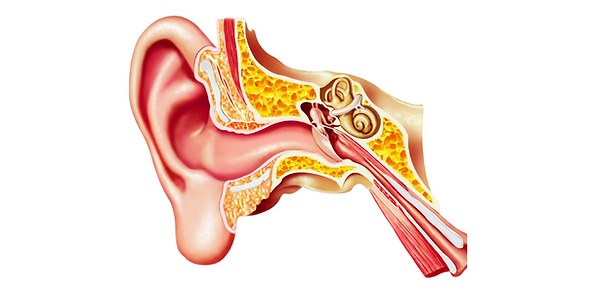
Are you experiencing itching, pain, or discomfort in your ear, particularly after swimming or exposure to moisture? These could be signs of Otomycosis, commonly known as Swimmer’s Ear. This fungal infection of the outer ear canal is a common condition, especially in humid climates or among swimmers. At my ENT clinic in Delhi, we offer effective treatment for Otomycosis, helping you get back to enjoying life without ear pain or discomfort.
Otomycosis is a fungal infection that affects the outer ear canal, often caused by prolonged exposure to moisture, which creates the ideal environment for fungi to thrive. While it’s commonly referred to as Swimmer’s Ear, it can also occur from other activities, such as bathing, showering, or excessive ear cleaning.
Fungal organisms like Aspergillus or Candida are the main culprits behind this condition. The infection leads to inflammation and irritation of the ear canal, resulting in a variety of symptoms.
The symptoms of Otomycosis can vary but typically include:
Itching or discomfort inside the ear
Redness or inflammation of the ear canal
Ear pain or a sensation of fullness in the ear
Drainage from the ear (may be thick and yellowish or clear)
Reduced hearing or muffled sounds due to the buildup of debris
Swelling of the ear canal or surrounding area
If left untreated, the infection can cause prolonged discomfort and may even lead to complications, especially if the fungus spreads to other parts of the ear or surrounding tissues.
Certain factors can increase the likelihood of developing Otomycosis:
Excess moisture: Swimmers or those who frequently immerse their heads in water are more prone to developing the condition.
Trauma to the ear canal: Using cotton swabs or other objects to clean the ear can scratch or irritate the ear canal, making it easier for fungi to invade.
Existing ear conditions: People with eczema, dermatitis, or other skin conditions around the ear are more susceptible.
Warm, humid environments: Living in or visiting areas with high humidity can encourage fungal growth.
Weak immune system: People with compromised immune systems are at higher risk of fungal infections.
If you suspect you have Swimmer’s Ear or Otomycosis, it’s important to seek medical attention promptly. An ENT specialist will:
Perform a visual examination of your ear using an otoscope to look for signs of infection and fungus.
Take a sample of the discharge from the ear canal for laboratory testing to confirm the type of fungus causing the infection.
The treatment for Otomycosis depends on the severity and type of fungal infection. Common treatment options include:
Antifungal ear drops – These are used to treat the infection and reduce inflammation and itching in the ear canal. Ear cleaning – A healthcare provider may clean out the ear canal to remove debris, discharge, or fungal growth and promote healing. Oral antifungal medication – In severe cases, oral medication may be prescribed to treat the infection more comprehensively. Pain relief – Over-the-counter pain medications or ear drops may be used to reduce discomfort during the healing process.
While Otomycosis is treatable, preventing it is even better. Here are some tips to protect your ears and reduce the risk of infection:
Dry your ears thoroughly after swimming or bathing. You can gently dry your ear with a towel or use ear-drying drops.
Avoid inserting objects like cotton swabs or fingers into your ears to prevent injury and irritation.
Use earplugs or a swimming cap to keep water out of your ears while swimming.
Keep your ears clean and dry, and avoid excess moisture or dampness in the ear canal.
If you experience any of the symptoms of Otomycosis, especially persistent ear pain, drainage, or itching that doesn’t improve, it’s important to see an ENT specialist for a diagnosis and appropriate treatment.
At my clinic in Delhi, we offer comprehensive care for Otomycosis, providing effective treatment and prevention strategies to help you avoid future ear infections.
How to Prevent Swimming Ear Infections in Children – Tips for Healthy Ears
As summer approaches, many children love to dive into the pool, spend time at the beach, or splash around in the water. However, these fun activities can sometimes lead to swimmer’s ear, also known as otitis externa, an ear infection that occurs when water gets trapped in the ear canal. If you’re a parent in Delhi concerned about your child’s ear health, this blog post provides expert tips on how to prevent swimming ear infections and ensure your child’s ears stay safe and healthy.
Swimmer’s ear is a common condition caused by moisture or bacteria in the ear canal. When water becomes trapped inside the ear, it creates an ideal environment for bacteria or fungi to grow, leading to an infection. Children are more prone to this type of ear infection because their ear canals are narrower, and they tend to spend more time in the water.
Symptoms of swimmer’s ear in children include:
Itching inside the ear
Ear pain or tenderness
Redness inside the ear canal
Fluid drainage from the ear
Difficulty hearing or a sense of fullness in the ear
If you notice any of these signs, it’s important to seek treatment promptly from an ENT specialist to avoid further complications.
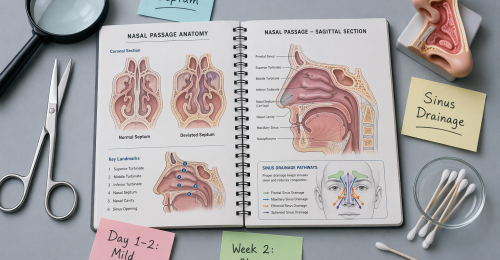
Breathing through your nose should feel effortless. But if you’re constantly dealing with blockage, sinus pressure, or difficulty sleeping because of poor airflow, it might not just be a temporary issue.
Conditions like a deviated septum or chronic sinus blockage can affect your daily comfort more than you realize. Procedures like Septoplasty and FESS (Functional Endoscopic Sinus Surgery) are designed to correct these problems and help you breathe better.
Let’s understand this in a simple and practical way.
Septoplasty is a procedure that corrects a deviated nasal septum — the thin wall inside your nose that separates both sides. When this wall is not straight, it can block airflow and make breathing difficult.
FESS (Functional Endoscopic Sinus Surgery) is used to open blocked sinuses and restore proper drainage using a small camera (endoscope).
In many patients, both problems exist together. That’s why these procedures are often done together for better, long-term results.
Many people get used to these symptoms and think they’re normal — but they’re not.
Not sure if these symptoms apply to you?
The septum may be off-center from birth or due to injury. When it shifts significantly, it can block airflow and make one nostril feel constantly congested.
Your sinuses need to drain properly. But due to:
…the drainage pathways get blocked, leading to pressure, discomfort, and repeated infections.
When both conditions exist together, symptoms tend to become more persistent.
Not every case needs surgery. Doctors usually start with medications. But if symptoms continue, surgery may be the next step.
Septoplasty and FESS are generally safe, but like any surgery, some risks exist:
No, it is done under anesthesia. Post-surgery discomfort is mild and manageable.
Improvement starts within 2–3 weeks as swelling reduces.
No, septoplasty focuses on breathing, not appearance.
Yes, though sinus care may still be needed.
Get expert evaluation and treatment guidance from an ENT specialist.
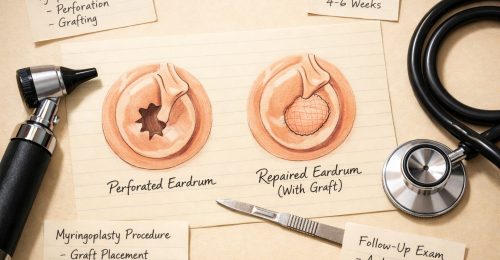
A perforated eardrum a hole or tear in the thin membrane separating your outer and middle ear is more common than many people realise. The good news: most perforations heal on their own, and when they don’t, effective treatments are available.
Consult Dr AashimaLearn More About Treatments
Disclaimer: This article is for general informational purposes only and does not constitute medical advice. Recovery timelines mentioned are typical estimates individual results vary. Always seek guidance from a qualified healthcare professional.
Symptoms depend on the cause, size, and location of the perforation. Some people notice a dramatic onset (such as after a loud blast or ear infection), while others discover the condition gradually.
Not sure if your symptoms match a perforation? A specialist can confirm with a simple ear exam.
The majority of small perforations particularly those caused by infection or minor trauma heal spontaneously within 4 to 8 weeks without any intervention. However, surgery becomes the appropriate path when:
Your ENT surgeon will assess perforation size (often using an otoscope or microscope), hearing test results (audiogram), and overall middle ear health before recommending surgery.
Endoscopic ear surgery has grown significantly in adoption over the past decade. By working entirely through the natural ear canal opening, it avoids the traditional post- auricular (behind-the-ear) incision, which means no visible scar and typically less postoperative discomfort.
However, there are limitations to be aware of:
Important: The “best” technique depends on your individual anatomy, perforation characteristics, and surgeon expertise not one approach suits all patients. Discuss options thoroughly with your ENT.
Wondering if endoscopic surgery is right for you?
Recovery varies depending on whether the perforation healed naturally or required surgery. The timelines below are typical estimates individual experiences differ.
An ENT specialist can confirm your diagnosis, discuss your treatment options, and guide you through the recovery process.
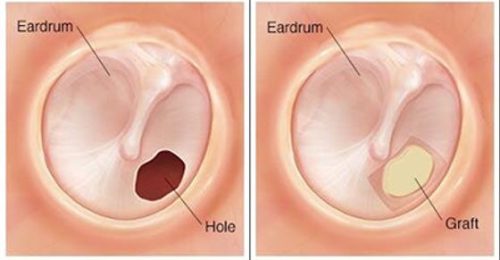
If you’ve been struggling with hearing loss, ear infections, or a perforated eardrum, Endoscopic Minimally Invasive Tympanoplasty may be the advanced solution you’re looking for. As an experienced ENT surgeon practicing in Delhi for over 10 years, I specialize in this cutting-edge, patient-friendly technique that offers excellent results with minimal discomfort and quicker recovery.
Endoscopic tympanoplasty is a modern surgical procedure used to repair a perforated eardrum (tympanic membrane) using a high-resolution endoscope. Unlike traditional microscopic surgery, this approach does not require large incisions or postauricular cuts. Instead, the entire procedure is done through the ear canal, making it truly minimally invasive.
No external incisions – No visible scars, as the surgery is done entirely through the ear canal.
Faster recovery – Patients usually experience quicker healing and less post-operative pain.
Improved visualization – The endoscope provides a wide-angle, high-definition view of the middle ear for more precise surgery.
High success rate – Proven outcomes in restoring hearing and closing eardrum perforations.
Ideal for children and adults – Especially effective in younger patients where minimal trauma is preferred.
This surgery is recommended for patients with:
Chronic ear discharge (chronic suppurative otitis media)
Hearing loss due to eardrum perforation
History of ear infections not responding to medical treatment
Eardrum injuries caused by trauma or pressure changes
Endoscopic tympanoplasty is revolutionizing how ENT surgeons treat middle ear conditions. By avoiding large cuts and improving surgical access, it offers a safer, faster, and more comfortable experience for patients. As someone trained and experienced in this advanced technique, I ensure personalized care tailored to each patient’s condition.
If you’re seeking a trusted ENT surgeon in Delhi for endoscopic tympanoplasty, my clinic ENT care clinic offers state-of-the-art care with a focus on patient comfort and optimal outcomes. Book a consultation today to learn how this minimally invasive ear surgery can help restore your hearing and improve your quality of life.